by admin | Aug 2, 2011 | Health Care Reform, healthcare, PPACA

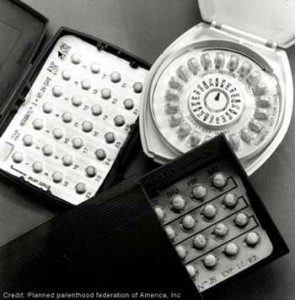
Under Health-Care Reform Insurance Coverage for Contraception Is Required – NYT; The Health Resources and Services Administration (HRSA), an arm of HHS, developed the women’s services package to implement the preventive health services provisions of the Patient Protection and Affordable Care Act of 2010 (PPACA).
Federal recommended that major medical plans should include coverage for:
- well-woman visits
- contraception
- screening for the viruses that cause AIDS and human papillomavirus
- breast-feeding support in the basic package of preventive health services benefits.
Health plans must roll this out by Aug 1, 2012. These are in accordance with the preventive care provisions enacted in the Reform Law. Agencies are determining what falls into this category and have amended this provision, see
here. While states such as NY already have these benefits built into their plan at no charge the medications are presently not free.
The contraception coverage requirement applies to drugs and devices approved by the federal Food and Drug Administration.
Exemption to religious organizations will be made available. This can be done at renewal time by groups’ broker. Unfortunately, non group individual policies will not allow for this exemption.
While this is a noble reccomendation, this is not as significant to NY and neighboring states. Some argue that the costs will indeed rise even in our region since the Rx will be free. Also, some consumers who currently purchasing supplies over the counter will tap into this free benefit.
Conclusion, not exactly a cost cutting decision as promised by the President to lower medical expenses but he did win over half the voters in time for next election!
![Health Reform: Grandfathering Your Current Insurance Plan (06/14/2010 Press Conference)]()
by admin | Aug 9, 2010 | group health insurance, Health Care Reform
[vodpod id=Video.4196761&w=425&h=350&fv=%26rel%3D0%26border%3D0%26]
“A promise to keep your health plan? …..Plans that existed on March 23 can make routine changes while remaining exempt form some of the new provisions. Americans who like their plan are extended security.” Really?
While there are a few small advantages the main advantage is for businesses with class-out situations where they have a Management vs. Non-Management plans. Industries commonly likely to get affected are medical offices, construction and restaurants. By using this clause they are afforded reprieve form non-discrimination. This affects groups renewing post Sept 23, 2010.
But how likely is allowing the Grandfathering Clause a benefit in real life situations. As per the attached June video press conference , if an insurance company decides to increase their costs sharing significantly they automatically lose this status. As an example, if an Oxford raises the deductible from $1000 to $1200 or by “15% + medical inflation rate”. Think this is unusual? Just check your benefits form 3 years ago and see if a $10 copay is still available.
 How about if a Healthnet decides to exit the Northeast market and sells to United Healthcare? Yes folks you’re out of luck.
How about if a Healthnet decides to exit the Northeast market and sells to United Healthcare? Yes folks you’re out of luck.
So what are the odds that small group will have this imposed on them? According to Gov Estimates the projections are 58%-80% in 2011 and dropping to 20%-51% in 2014 still remaining grandfathered. When calculating small employees the number is less than 100 employees. I suspect for groups under 50 employees the numbers are further skewed.
Which is why in summation this is a red herring issue and wont pose as a viable advantage for most groups. An excerpt below form our Crains interview earlier this summer discusses the Grandfathering Clause further.
“The prohibition on changing carriers, in particular, takes an important cost-control tool away from small businesses, which already lack the flexibility and leverage of larger companies. Many change carriers every couple of years in search of better rates or new offerings as insurers offer deals to drum up new business. Westchester broker Alex Miller says that for most of his small business clients, trying to keep their grandfathered status is probably not worth it, especially if rates continue to climb 15% to 20% a year as they have in New York. With limits on cost-sharing, employers could get further behind every year.
“I think a small handful of my clients will stay put because they have a unique health care plan, such as an indemnity plan that is no longer sold,” says Mr. Miller, president of Millennium Medical Solutions Corp. in Armonk. “But for the great majority of my clients, how are they going to take a 20% [premium] increase and not make any changes?””


