by Alex | Apr 20, 2016 | healthcare, Individual Exchanges, individual health insurance, latest health insurance news, Obamacare, State Exchanges, United Healthcare
UnitedHealthcare will drop ACA exchanges
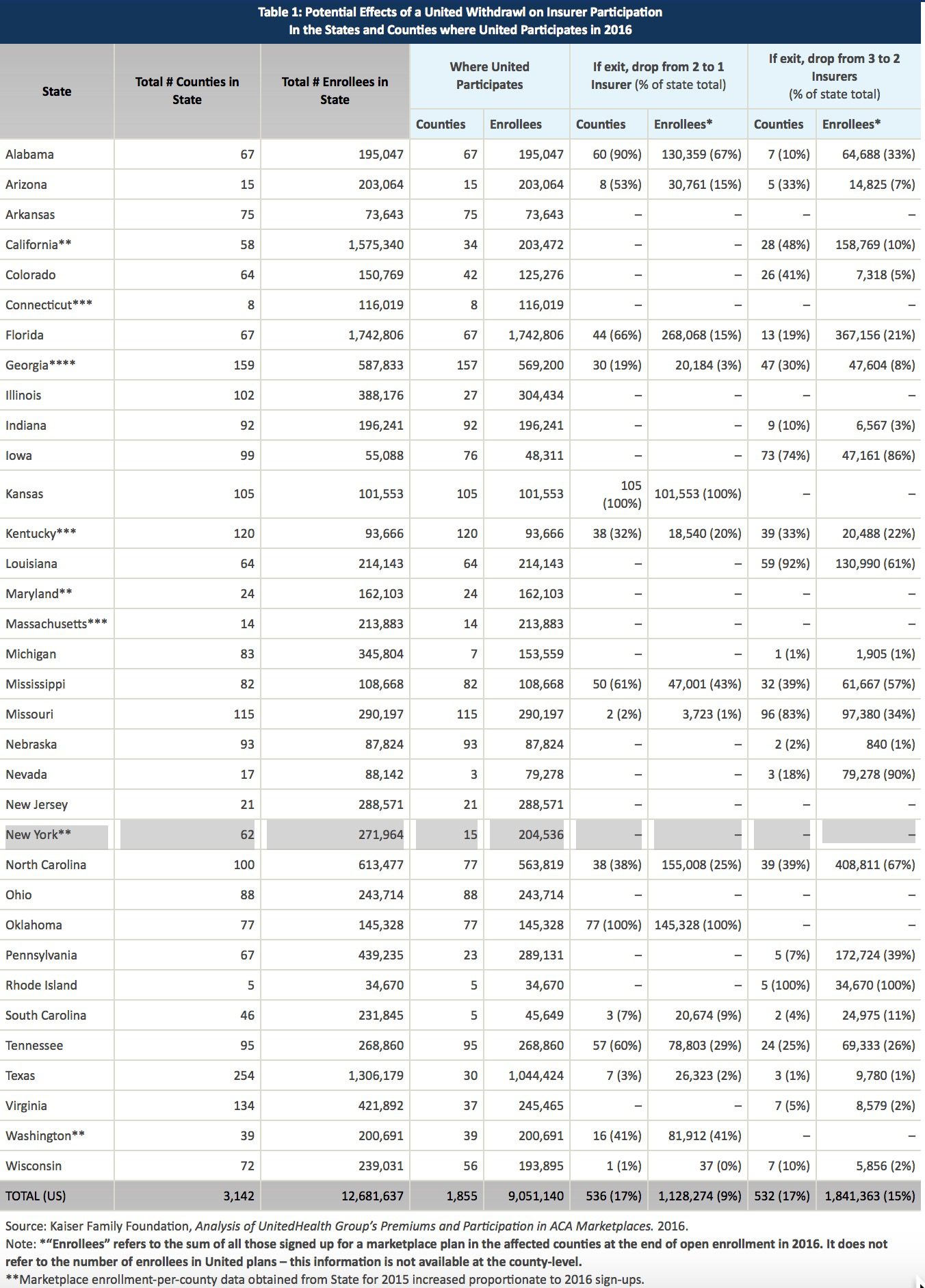
UnitedHealthcare Individual by State
BREAKING:
So far, New York and Nevada have confirmed that UnitedHealth plans to remain on their ACA exchanges next year. The company has also filed plans to participate in Virginia for 2017. Wisconsin said it hasn’t received an exit notice from UnitedHealth, and that it doesn’t comment on insurers’ business plans. A representative of Covered California, the state’s Obamacare exchange, said plan participation is confidential until it’s announced later this year.
UnitedHealthcare will drop out of most ACA Exchanges by 2017 as reported in Modern Healthcare. Just how significant is this to the market? Realistically, United took a cautious wait and see approach. In NYS, for example, they have been the most expensive plan on the Obamacare Exchange Marketplace. They expect to lose over a billion dollars in this space for 2015 and 2016, so to them it makes no sense to stay in that market. The concern for the individual market is to expect large pricing increases in 2017 to reflect the higher risk than the safer Group Market.
UnitedHealth, which had about 795,000 ACA customers as of March 31, warned in November that it was posting losses on ACA policies. In December, the company said it should have stayed out of the individual exchange market longer. UnitedHealth also is withdrawing from some related state insurance markets for small businesses.
See United-healthcare Individual members enrolled by State: 
UnitedHealthcare will drop ACA exchanges
MODERN HEALTHCARE
By Bob Herman
April 19, 2016
UnitedHealth Group CEO Stephen Hemsley said Tuesday the health insurance and services conglomerate will pull out of most of its Affordable Care Act marketplaces. But the company won’t bail on the exchanges completely and will sell individual plans in a “handful” of states.
“We cannot broadly serve it on an effective and sustained basis,” Hemsley told analysts and investors on a conference call. UnitedHealth has fully or partially exited five states so far—Arkansas, Georgia, Louisiana, Michigan and Oklahoma, according to various news reports.
The company sold plans in 34 states for this policy year and did not disclose which states it will stay in. Insurers that sell plans through the federal HealthCare.gov portal have until May 11 to file rates for 2017 plans.
A new analysis from the Kaiser Family Foundation, however, notes that UnitedHealth’s exits would only have a modest effect on competition and prices nationally since it has a small ACA footprint and charged higher premiums from the outset.
UnitedHealth recorded an additional $125 million loss on its individual ACA plans, meaning the company’s total ACA losses for 2015 and 2016 will exceed $1 billion. UnitedHealth signed up many sicker-than-expected members, ending the first quarter with 795,000 public exchange enrollees, which is only a fraction of the ACA’s individual market.
The insurer also overpriced its plans in 2015 after barely participating on the exchanges in 2014. UnitedHealth expects its exchange membership will decline to 650,000 by the end of the year.
But despite those heavy losses, which UnitedHealth previewed late last year, the company’s other lines of business like Medicare Advantage and Optum have been making money at a healthy clip. UnitedHealth’s profit climbed 14% year over year, totaling $1.6 billion in the first three months of this year. Adjusted earnings per share rose 17% to $1.81, beating estimates on Wall Street.
Revenue soared almost 25% to $44.5 billion in the first quarter, putting UnitedHealth on pace to hit $182 billion of revenue for the year. The Minnetonka, Minn.-based company recorded double-digit revenue growth across every major segment, including employer, Medicaid, Medicare Advantage and its Optum health services business. UnitedHealth now covers the medical care of nearly 47.7 million Americans.
UnitedHealth’s medical-loss ratio, which shows how much of its premium dollars were spent on medical care or “quality improvement” programs, was 81.7% in the quarter. That was up slightly from the 81.4% posted in the same quarter last year, which UnitedHealth attributed to the leap day.

by Alex | Oct 30, 2015 | Health Care Reform, Health Exchanges, Individual Exchanges, individual health insurance, latest health insurance news, NY News, Obamacare, regional health insurance co-ops, State Exchanges
 Health Republic NY Shutting Down Nov 30
Health Republic NY Shutting Down Nov 30
Breaking: All Health Republic plans (Group and Individual) ending on 11/30. according to early reports the healthcare Co-Op Health Republic NY will be shutting down Nov 30, 2015. New York State Department of Financial Services (NYDFS), the New York State of Health Marketplace (NYSOH), and the Centers for Medicare and Medicaid Services (CMS) announced additional actions regarding Health Republic Insurance of New York (“Health Republic”) and a transition plan for Health Republic customers.
TIMELINE:
- Oct 28th – Utah Healthcare Co-Op shutting down end of 2015. This sis the 5th Co-Op to shut down

- Sept 25, 2015 – original announcement Health Republic NY is Shutting Down effective Dec 31, 2015.
- June 2015 – With a spike in rate increase of 15-20% for 2016 to reflect unexpected high costs of new 200,000 membership the most affordable health plan was experiencing difficulties. The insurer reported $130 million in losses during its first 18 months of operations, according to financial filings, even as it enrolled more customers than any other insurer. DFS did allow for a 13 percent increase in the second year and a 14 percent increase heading into 2016. Both were lower than what Health Republic requested, though, and were not enough to save the struggling insurer.
- May 2015- Health Republic was dealt its death blow when it became clear that the Affordable Care Act’s risk corridor program would not be fully funded, said one source familiar with the company’s finances. A report from Standard & Poor’s in May said the program had only 10 percent of the funds needed to make payments.
- Summer 2013 -Health Republic had borrowed $265 million to begin operations.
New Insurance Risk Corridors paid for by a combination of both consumer insurance premium surcharge tax of 2-3% and Health Insurers is suppose to reclaim capital to those that are less profitable. Health Republic was owed approximately $147 million but was told by the Centers for Medicare and Medicaid Services to expect less than half that according to sources.
Regrettably, we all suffer when an Insurer exits the market. Furthermore, it will be a while again when Federal funds earmarked to start a low cost affordable health plans will materialize again. We are pulling for neighboring co-op Health Republic of NJ and hope this trend discontinues.
Our agency will be working closely with our clients to mitigate this exposure and transition smoothly for Dec 1, 2015. Individuals on the Marketplace can contact the New York State Department of Financial Services Consumer Hot Line with questions regarding Health Republic by calling 1-800-342-3736. The Hot Line hours are weekdays (Monday through Friday) from 8:00 a.m. to 8:00 p.m., and Saturday from 9:00 a.m. to 1:00 p.m.
Please Click here to read the full Press Release from NYDFS.
Stay posted, more news to follow. Our Agency as in the past will be out and early in front positioning our clients for best options. For more information on this or to schedule a call please contact us info@medicalsolutionscorp.com today.

by Alex | Oct 20, 2015 | Health Exchanges, Individual Exchanges, individual health insurance, Obamacare
2016 Individual Open Enrollment Deadlines:
- November 1, 2015: Open Enrollment starts — first day you can enroll in a 2016 insurance plan through the Health Insurance Marketplace. Coverage can start as soon as January 1, 2016.
2016 plans and prices will be available for preview the third week of October, 2015.
- December 15, 2015: Last day to enroll in or change plans for new coverage to start January 1, 2016.
- January 1, 2016: 2016 coverage starts for those who enroll or change plans by December 15.
- January 15, 2016: Last day to enroll in or change plans for new coverage to start February 1, 2016
- January 31, 2016: 2016 Open Enrollment ends. Enrollments or changes between January 16 and January 31 take effect March 1, 2016.
If you don’t enroll in a 2016 health insurance plan by January 31, 2016, you can’t enroll in a health insurance plan for 2016 unless you qualify for a Marketplace Special Enrollment Period.
Penalty: The uninsured penalty rises to $695 or 2.5% of your income, whichever is higher.
Coverage start dates
If you enroll before the 15th of any month, your coverage starts the first day of the next month. If you enroll after the 15th of the month, you’ll have to wait until the month after that for your coverage to start. So, for example, if you enroll on January 16, your coverage would start on March 1.
Enroll using our online comparison shopping tool for both on and off-Exchange Marketplace to be released next week. Email us or Contact us at (855)667-4621.

by Alex | Oct 18, 2015 | group health insurance, Health Exchanges, Healthy NY, Individual Exchanges, individual health insurance, NY News, Uncategorized

NEW 2016 Oxford Metro Network NY
Oxford has released an affordable new plan for 2016 and not a moment too soon. With the recent exit of popular Health Republic of NY, Health Republic NY is Shutting Down, the market is starving for an affordable option.
Today’s largest networks with in-network only GOLD are priced at $9,000/single annually. They typically are accompanied with $50 copays and non-office exposures of $1,000 deductibles and coinsurance percent in network. The new Metro network is approximately 25% smaller than NY Liberty network with up to 15% IN SAVINGS. For example, an Oxford Liberty HMO Gold is $745 vs Oxford Metro Gold $650.
In 2015 Oxford’s Garden State Network originated the same game plan of offering a third network in addition to FREEDOM and LIBERTY. After all what good is a large network when one cannot afford to visit Providers? The third network answers the call for access to Providers with half the copays priced at approximately $1,500 less.
All Metal Levels will be included for all size groups including 1-99 & 100+. The new Oxford Metro plan will be limited to NY and NJ Garden State Network Providers. Referrals will be needed to see Specialists. Importantly, most NY Hospitals will be participating with the EXCEPTION of NYU Health System, North Shore LIJ Health System (NorthWell Health) and Maimonides Medical Center. In addition, certain key medical IPA Groups such as Mt Kisko Medical Group are NOT in the network.
The Healthy NY and off-exchange Individuals will use exclusively this new Oxford Metro Network.
DOCTOR SEARCH: Click Here
BENEFITS SUMMARY: OXFORD Platinum, Gold, Silver AND Bronze
Individual Sample Rates: Oxford 2016 NY Individual Rate Sheet
Individual Enrollment Forms: Oxford 2016-NY-MMS-Individual-application-Kit
Individual ON-Exchange UHC Network
Oxford Drug Formulary: Click Here
Oxford Metro FAQ. Click Here
Group Sample Rates:
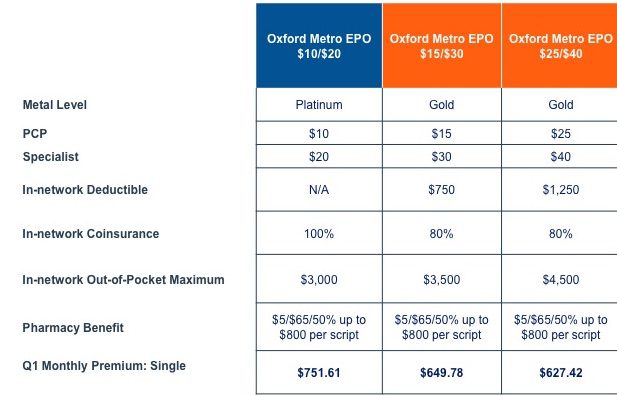
Platinum & GOLD
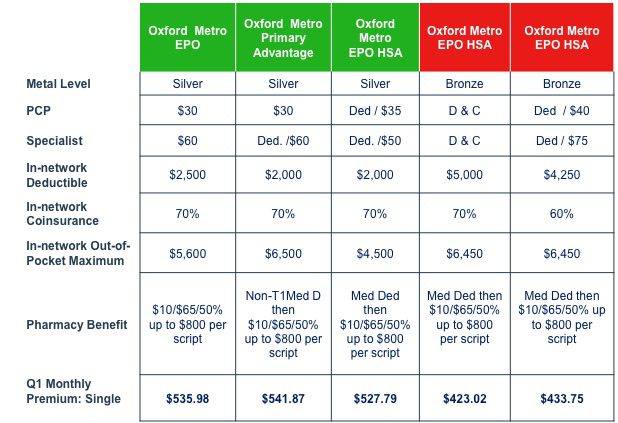
Silver & Bronze
3 steps:
1. Initial Check Deposit: “Oxford Health Plans”.
2. Proof of address:
- Valid New York State driver’s license
- Voter Registration Card
- Current income tax return, current lease or current utility bill
- If mailing address is different than street address, please provide mailing address under separate cover
3. Enrollment form below and mail back to:
Oxford Individual Product Department
14 Central Park Drive
Hooksett, NH 03106
NOTE: Jan 15th deadline to submit Feb 1, 2016 effective date. Jan 31st is the deadline for a March 1, 2016 effective date.
Sign up for upcoming webinars and newsletters. Please contact us TODAY for a customized analysis for your group-specific needs at info@medicalsolutionscorp.com or Call (855) 667-4621.
by Alex | Oct 12, 2015 | group health insurance, Health Exchanges, Individual Exchanges, individual health insurance, NY News, Obamacare
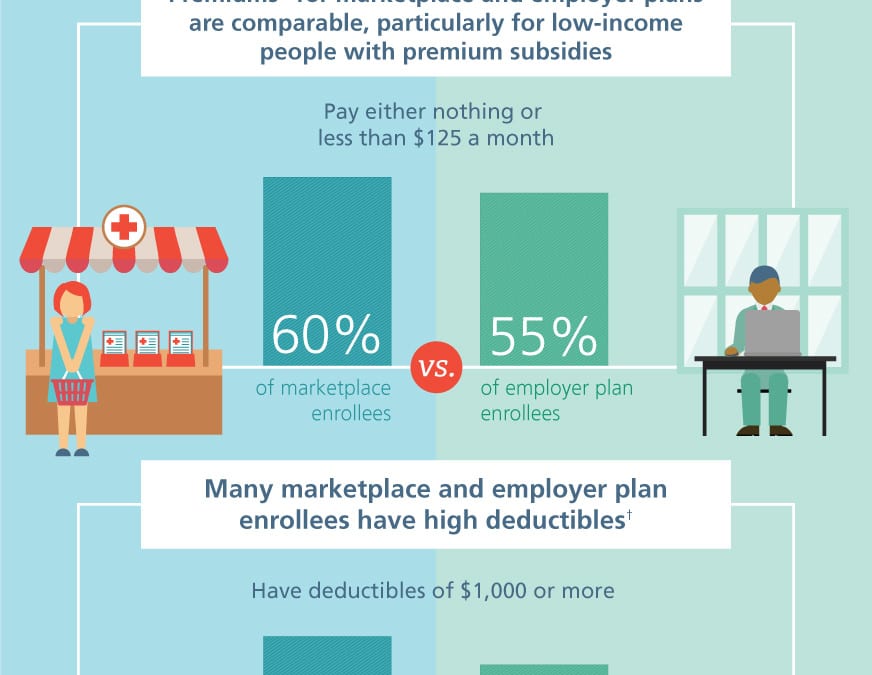
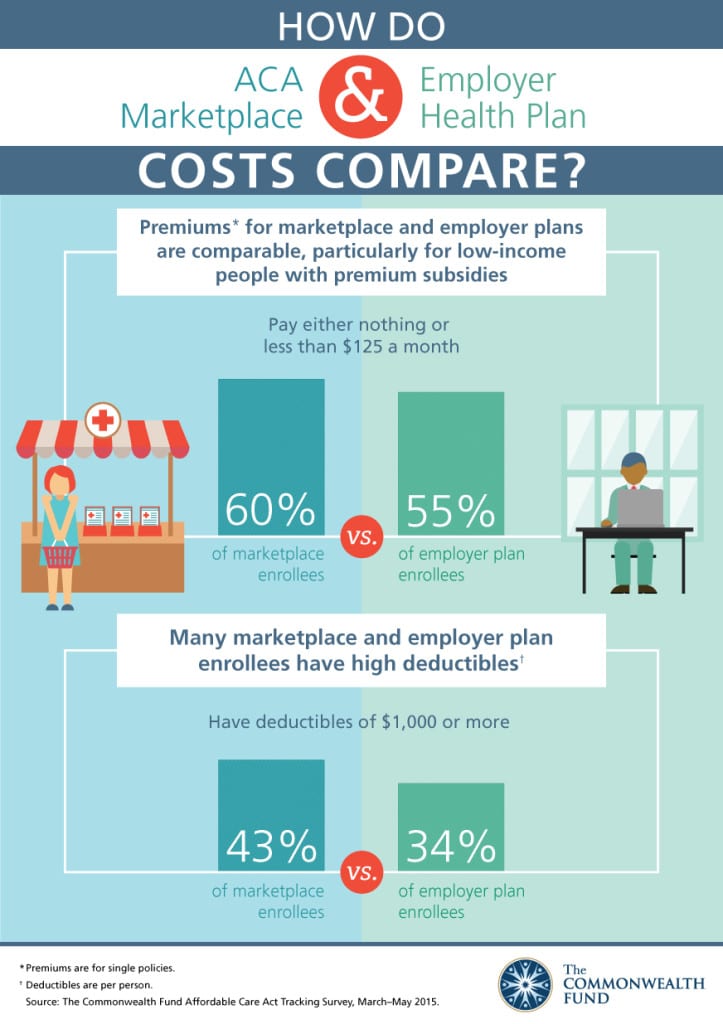
ACA Marketplace and Employer Health Plan Cost Comparison
Are you ready for 2016 Individual Open Enrollment? The #1 question we get form individuals is am I better off staying on the individual plan or joining my small employer group plan?
Starting Nov 1, 2015, the 3rd anniversary of Obamacare’s ACA Marketplace begins. Continuing through 2018, several new parts of the Affordable Care Act that affect costs and benefits will be rolled out. The remaining provisions will take effect against a backdrop of new patterns in health care spending and trends.
A frequent Employer question is how do costs compare on the ACA Marektplace vs. Employer Health Plans. The infographic from the Commonwealth Fund point out that the premiums are more favorable when factoring low income premium subsidies. In order to even the scales, an individual must earn $23,500 for a net subsidized premium of $125/month (click Kaiser calculator). This number represents 60% of marketplace enrollees. The same $125/month contribution amount represents 55% of employer health plans.
One positive point is that U.S. health care spending has slowed in the past few years. In a recent 16-month period, nearly 23 million Americans have enrolled in the Affordable Care Act, while almost 6 million people lost coverage. Research from Rand Corp. finds that of the newly insured:
- 42 percent are covered through employer-sponsored plans.
- 29 percent are enrolled in Medicaid.
- 18 percent have health coverage in individual marketplaces.
Take a look at the infographic:
2016 Open Enrollment Deadlines:
- November 1, 2015: Open Enrollment starts — first day you can enroll in a 2016 insurance plan through the Health Insurance Marketplace. Coverage can start as soon as January 1, 2016.
FYI2016 plans and prices will be available for preview the third week of October, 2015.
- December 15, 2015: Last day to enroll in or change plans for new coverage to start January 1, 2016.
- January 1, 2016: 2016 coverage starts for those who enroll or change plans by December 15.
- January 15, 2016: Last day to enroll in or change plans for new coverage to start February 1, 2016
- January 31, 2016: 2016 Open Enrollment ends. Enrollments or changes between January 16 and January 31 take effect March 1, 2016.
If you don’t enroll in a 2016 health insurance plan by January 31, 2016, you can’t enroll in a health insurance plan for 2016 unless you qualify for a Marketplace Special Enrollment Period.
Penalty: The uninsured penalty rises to $695 or 2.5% of your income, whichever is higher.
Coverage start dates
If you enroll before the 15th of any month, your coverage starts the first day of the next month. If you enroll after the 15th of the month, you’ll have to wait until the month after that for your coverage to start. So, for example, if you enroll on January 16, your coverage would start on March 1.
Enroll using our online comparison shopping tool for both on and off-Exchange Marketplace to be released next week. Email us or Contact us at (855)667-4621.

by admin | Jun 25, 2015 | Health Care Reform, Health Care Refrom, Individual Exchanges, Obamacare, State Exchanges

Supreme Court Upholds ACA Again
The U.S. Supreme Court ruled this morning that the Affordable Care Act may provide nationwide tax subsidies for people who purchase health insurance through an exchange. The Court considered a challenge to a provision of the ACA concerning whether subsidies were available only to those who purchased health insurance on an exchange “established by the state.” The Court, in King v. Burwell, ruled 6 to 3 in favor of upholding the eligibility for people to receive subsidies through either a state or federal health insurance exchange.
The opposite ruling would have had serious implications for the country due to the number of states relying on a federally-run exchange (37 states) and the number of customers who qualify for subsidies based on their income (about 85% of customers nationwide). The Government’s argument prevailing: defending the subsidies, the Government argued that if you look at the entire ACA and its history, it is clear that the subsidies are available to everyone who purchases insurance on an exchange, no matter who created it.
Please join us for upcoming Webinar on How to Prepare for Current and Future ACA Requirements.

Are you able to identify and address all of the ACA requirements? Have you developed a plan of action to help stay in compliance? This webinar will walk you through a three year case study and provide you with current and future solutions to help your group prepare for ACA challenges including the Cadillac Tax.
Some of the key webinar highlights include:
- Will Federal subsidies stop in some states making residents unable to access subsidized Exchange coverage?
- 3 year case study providing a practical view
- Will IRS information reporting still be required?
- Could Congress step in and propose changes to the existing ACA law?
- 2015 – Section 125 changes including eligibility, PRAs, excepted benefits and FSA plans for higher OOP exposure
- 2016 – Renewal focus on HSA’s with a dollar for dollar matching contribution
- 2017 – Further conversation of reducing benefit costs utilizing post deductible HRA’s and consideration of Defined Contributions
Practical information you can use – a webinar you will not want to miss!












